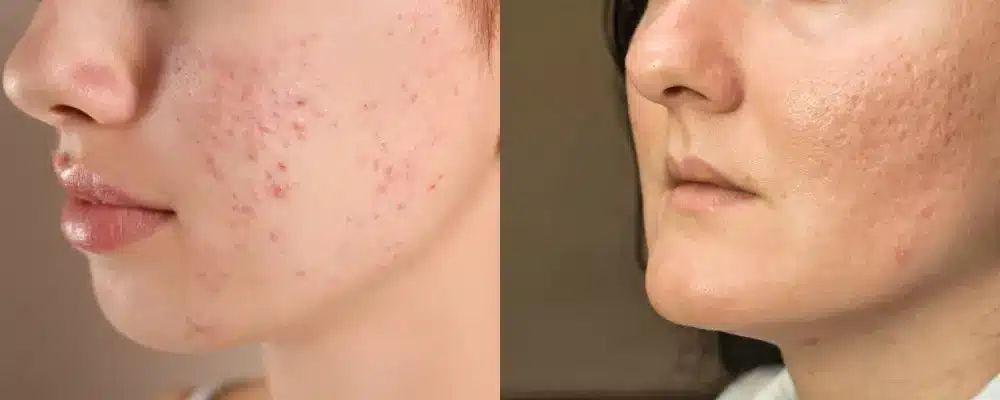
Acne is a common skin condition affecting both teenagers and adults. While active acne may eventually settle, it can leave behind permanent scars that affect skin texture, appearance, and confidence. Understanding what acne scars are and how they form is critical for effective treatment and long-term skin health.
Acne scars are structural changes in the skin resulting from damage to the dermis, the deeper layer of the skin responsible for strength and elasticity. They differ from post-inflammatory hyperpigmentation (PIH), which affects skin color rather than structure. PIH can fade over time or with topical treatments, but true acne scars are permanent changes in skin architecture and do not resolve on their own.
The Biology Behind Acne Scar Formation
Acne scars form as a result of abnormal wound healing. Severe inflammation from acne lesions triggers a cascade of repair processes, but disruptions in this process can lead to permanent structural changes.
The Wound-Healing Process
- Inflammatory Phase
- Immune cells rush to the site to eliminate bacteria and damaged tissue.
- Excessive or prolonged inflammation can destroy collagen and elastin fibers in the dermis, which are essential for skin strength and elasticity.
2. Proliferative Phase
- Fibroblasts produce collagen to rebuild the dermal matrix.
- When collagen deposition is disorganized, scars or irregularities begin to form.
3. Remodeling Phase
- Collagen continues to reorganize over weeks to months.
- Abnormal remodeling can lead to indentations (atrophic scars) or raised scars (hypertrophic/keloid scars).
Severity and duration of inflammation are major determinants of scar formation. The longer acne lesions persist, the more damage occurs in the dermis, increasing the likelihood of permanent scarring.
Factors Influencing Acne Scar Formation
Not everyone with acne develops scars. Certain factors increase the risk:
- Severity and type of acne – Nodulocystic or deep inflammatory acne is more likely to damage dermal structures.
- Delayed or inadequate treatment – Persistent inflammation increases dermal destruction.
- Genetic predisposition – Some individuals produce excessive collagen (hypertrophic/keloid scars) or insufficient collagen (atrophic scars).
- Skin type and ethnicity – Malaysian skin (Fitzpatrick III–V) is more prone to post-inflammatory hyperpigmentation, which may make scars appear more pronounced.
- Mechanical trauma – Picking, squeezing, or scratching acne lesions increases tissue injury.
Hormonal factors – Androgen fluctuations can increase inflammation and sebum production, indirectly contributing to scar formation.
Types of Acne Scars: Detailed Overview
Acne scars vary in structure, depth, and appearance. Accurate classification is essential to choose effective treatment.
1. Atrophic Scars
Atrophic scars result from collagen loss, leaving depressions in the skin. They are the most common facial scars.
a. Ice Pick Scars
- Appearance: Narrow (<2 mm), deep, and sharply defined pits.
- Cause: Severe localized inflammation that destroys a small volume of dermis.
- Clinical note: These scars extend deep into the dermis, making them challenging to treat.
- Common in: Cheeks and perioral area.
b. Boxcar Scars
- Appearance: Wider depressions (1.5–4 mm), with steep edges and flat bases.
- Cause: Broader areas of dermal destruction during inflammatory acne.
- Clinical note: Often mistaken for aging lines, but they are permanent without treatment.
- Common in: Cheeks and temples.
c. Rolling Scars
- Appearance: Wave-like, uneven texture due to fibrotic bands pulling the skin downward.
- Cause: Fibrous tissue forms under the skin, tethering the dermis to subcutaneous layers.
- Clinical note: Can make skin appear rough and uneven; often best treated with subcision combined with resurfacing.
- Common in: Cheeks and jawline.
2. Hypertrophic and Keloid Scars
- Hypertrophic scars remain within the boundaries of the original lesion and are caused by excess collagen production.
- Keloid scars extend beyond the original lesion, forming thick, raised tissue.
- Mechanism: Overactive fibroblast activity during wound healing produces excessive collagen.
- Clinical note: Less common on the face but prevalent on the jawline, chest, and shoulders.
- Risk in Malaysian skin: Medium to darker skin tones have a higher propensity for keloid formation.
3. Post-Inflammatory Hyperpigmentation (PIH)
- Appearance: Flat, darkened patches or spots.
- Cause: Melanin overproduction in response to inflammation, not structural dermal damage.
- Clinical note: Often coexists with scars, creating the appearance of more severe scarring.
- Treatment: Responds to topical lightening agents, sun protection, and sometimes laser therapy.
4. Mixed Scar Types
- Many patients present with more than one type of scar, requiring combination treatments.
- Example: A patient may have ice pick scars on the cheeks, rolling scars near the jawline, and pigmentation from prior inflammatory lesions.
- Clinical implication: Proper classification is crucial for effective planning.
How Scars Differ From Normal Healing
Normally, after mild acne, the skin heals with organized collagen deposition, leaving a smooth surface. Scars occur when this repair process is disrupted:
- Underproduction of collagen → atrophic scars
- Overproduction of collagen → hypertrophic/keloid scars
- Fibrotic tethering → rolling scars
- Persistent inflammation → hyperpigmentation
Essentially, scars are the result of imbalances in the wound-healing process, and each type reflects a distinct pattern of tissue repair gone awry.
Role of Inflammation and Depth
The depth of acne inflammation determines the likelihood of scarring:
- Superficial lesions (epidermis) usually heal without scarring.
- Deep lesions (dermis involvement) destroy collagen and elastin, resulting in permanent structural changes.
- Prolonged inflammation intensifies tissue destruction and increases the risk of multiple scar types.
Importance of Early Intervention
- Early acne treatment reduces inflammation duration and dermal damage.
- Professional intervention helps prevent deep scarring before lesions heal improperly.
- Educating patients to avoid squeezing or picking lesions can significantly reduce scarring.
Even after scars have formed, understanding their type and formation mechanism allows clinicians to select the most appropriate treatment and set realistic expectations.
Conclusion
Acne scars are permanent structural changes caused by abnormal wound healing following inflammatory acne. They can manifest as:
-
Atrophic scars: ice pick, boxcar, rolling
-
Hypertrophic/keloid scars: raised and thickened lesions
-
Post-inflammatory hyperpigmentation: dark marks without structural changes
Key points:
-
Not all acne leads to scarring; risk increases with severe, untreated acne, genetic factors, and mechanical trauma.
-
Malaysian skin types may develop pigmentation alongside scars, requiring careful management.
-
Accurate scar classification is essential for effective treatment planning.
-
Early intervention, proper acne management, and avoiding lesion trauma reduce long-term scarring.
By understanding how acne scars form, patients and clinicians can choose targeted, effective treatments and achieve meaningful improvements in skin texture and appearance.
Frequently Asked Questions
1. What causes acne scars on the skin?
Acne scars are caused by damage to the deeper layer of the skin (dermis) during severe or prolonged inflammatory acne. When the skin heals abnormally, it can result in indented, raised, or pigmented marks that are permanent and affect skin texture.
2. How do acne scars form?
Acne scars form when the skin’s natural wound-healing process is disrupted. Severe or prolonged inflammation from acne destroys collagen and elastin, and abnormal repair can result in:
-
Loss of collagen → atrophic scars
-
Excess collagen → hypertrophic or keloid scars
-
Fibrotic tethering → rolling scars
3. What are the main types of acne scars?
The three main categories are:
-
Atrophic scars: ice pick, boxcar, and rolling scars caused by collagen loss or fibrotic bands
-
Hypertrophic and keloid scars: raised scars caused by excessive collagen production
-
Post-inflammatory hyperpigmentation (PIH): flat dark marks often seen alongside scars, caused by excess melanin, not structural damage
4. Who is at risk of developing acne scars?
Scarring risk increases with:
-
Severe or prolonged acne (especially nodulocystic acne)
-
Delayed or inadequate acne treatment
-
Picking or squeezing lesions
-
Genetic predisposition to abnormal collagen formation
-
Malaysian skin types (Fitzpatrick III–V), which are prone to pigmentation alongside scarring
5. Can acne scars heal on their own?
No. While mild pigmentation may fade over time, true acne scars do not resolve naturally because the dermal structure is permanently altered. Effective treatment typically requires procedural interventions tailored to the type of scar.
6. Why is early acne treatment important for preventing scars?
Early medical intervention reduces inflammation duration and limits dermal damage. Proper acne management combined with avoidance of picking or trauma can significantly lower the risk of permanent scarring. For existing scars, early evaluation helps clinicians design targeted treatment plans for optimal results.

